The Long Haul
Battling long COVID, a science writer and entomologist tries to understand what is happening to an overlooked specimen — herself. Photography by Joshua Steadman.

By Eleanor Spicer Rice ’03, ’12 PHD
For weeks, I’d been on the receiving end of blaring horns. “That man just gave us the middle finger!” my 7-year-old reported daily from the back seat. In this “post-COVID” world, I was pretty sure drivers had lost their minds.
It wasn’t until I had an adult passenger in the car, my father, that I understood: Something’s not right about my reality.
As I waited patiently for the light to change green and then drove through the intersection, I heard those horns and noticed my father had adopted the posture he used when I was first learning to drive, right foot on the imaginary passenger side brake, one hand braced on the dashboard, the other grasping for support in the direction of the window. “What color do you think that light is, Eleanor?”
I looked up as we passed under it. It was red. How did it turn red so fast? It was green just a second ago! My father gently explained that I had stopped for the green light, which looked like a normal red light to me. Then, when it changed to red, I drove right on through, to the bewilderment and frustration of the drivers around me.
This was December 2021, three months into my long COVID journey. This was when I quit driving without an adult in the car.

Suppose those inspirational posters are right, and every challenge really is a learning opportunity. I was living in one of the strangest challenges of my life, a great nesting doll of challenges, each with another inside of it. By this point, I’d lost my voice, my memory, my sense of self, my ability to read or thermoregulate or sleep at night, or walk more than a block. I’d lost the ability to get my children ready for school, my breath, my feeling in my right arm and now my ability to drive. I’m 41 years old and otherwise active and healthy. I’ve never experienced long-term illness like this in my life. As someone with a keen interest in science — I have a Ph.D. in entomology and work as a science writer — I felt eager to find as much information about my condition as I could. As a mother of two children, ages five and seven, I was desperate to return to my former self as quickly as possible. I wanted to walk them to school. I wanted to be able to pick them up to kiss them when they fell. But long COVID remains hazily understood, refusing to operate on any timeframe except its own.
. . . long COVID remains hazily understood, refusing to operate on any timeframe except its own.
Six months into long COVID, I’ve experienced what it’s like to stare into a chasm, unable to see the other side. Navigating the long COVID abyss, I’ve come to understand that there are lessons nestled in challenges. I’m still making sense of some of them. Others I’ve had time to work through.
Long COVID is something. When I first experienced symptoms of long COVID, a.k.a. “long-haul COVID,” “post-acute COVID-19,” “long-term effects of COVID,” “chronic COVID,” or “Post-Acute Coronavirus Disease Syndrome,” I didn’t know it was an actual thing.
I was fully vaccinated when I got a positive test result back in August 2021. Having COVID wasn’t the best four days of my life, but according to Google, my symptoms fell solidly in the “mild-to-moderate” category.
However, even after I tested negative, I wasn’t getting better. Walking downstairs from my bedroom was an ordeal. My heart raced. I gasped for breath as if I’d just run a marathon. “Don’t wait on me,” I’d wheeze, with a voice that sounded like Don Corleone from The Godfather, except the only offer I’d make that my family couldn’t refuse was to scoop me up off the floor.

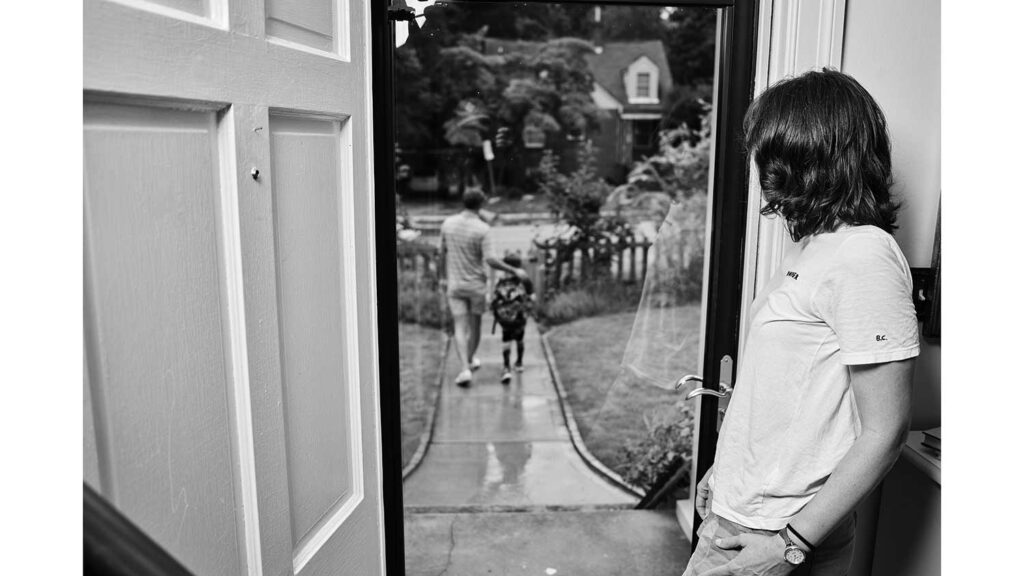
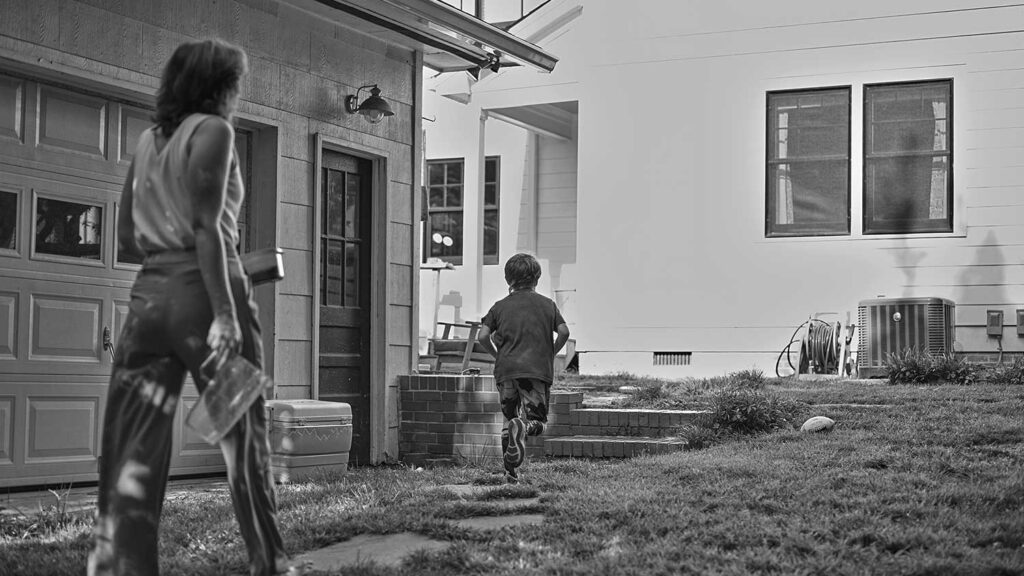
I couldn’t walk my son to school in the morning even though the school is a block from our house. A parent called to check on me. “Are you a long-hauler?!” she asked when she heard my voice. “Long-hauler” was a term that had just hit the news cycles that week. Little was known about it. I’d never heard the term before. How dare she! I’m not a one-woman super spreader!
I couldn’t walk my son to school in the morning even though the school is a block from our house.
“I’M . . . TESTING . . . NEGATIVE!” I wheezed.
But I was a long-hauler. And so are up to 30 percent of people who test positive for COVID. Even by the most conservative estimates, millions of people in the United States are living with long COVID. We’re not sure why some people get on with their lives while others are left to manage symptoms lasting weeks, months, or longer. Still, it’s real.
Long COVID offers an assortment of trouble for anyone under its spell. My mother and I pulled into my aunt and uncle’s driveway in my hometown of Goldsboro, N.C., for Thanksgiving supper, a week or two before I realized I was a hazardous driver. My mother switched off the car and offered some advice: “When someone asks you how you’re feeling, why not just say, ‘I’m recovering.’ You don’t have to say every single thing that is wrong with you right now.”
As with many chronically ill people, I spent so much time with my symptoms that they were one of the only things I wanted to discuss. I would talk — and talk — about my symptoms, in part because I was hoping someone would tell me what was wrong with me, or tell me I was normal, or at the very least tell me that it all sounded horrible to them, too.
The answer to, “How are you feeling these days, Eleanor?” would go something like this:
“I have these recurring fevers that last a few hours or a few days. Sometimes I can’t really breathe, and I don’t know why. I can’t remember things, like whole days or sometimes weeks, and sometimes it’s stuff that happened recently and sometimes it’s people from my past. I lost a bunch of hair, and sometimes I sit up at night going down these unstoppable doom spirals. My eyeballs changed shape for a couple of weeks, but they’re fine now. My arm is numb. I cry a lot. Do you think I’ll get better?”
Though I had little social wherewithal when it came to long COVID, I did have enough awareness to see that people would look concerned, then uncomfortable, then in search of an exit.
Long COVID may be caused by a number of factors. One possible factor is cell damage. The COVID virus kills the cells of infected people, which could result in lingering symptoms wherever those cells were killed. It could cause a rapid heartbeat in people who had heart damage. It could cause cognitive issues in people with brain damage.
Even if someone has recovered from COVID, the virus may linger in their organ tissue, which could cause a cascade of effects. The immune system, knocked off balance by the virus, could be weakened, resulting in the activation of other viruses sleeping in the body.
Like many things in life, the truth is probably found in a combination of pathways. COVID recovery clinics are popping up across the country to try to find some answers or at least clues. I am under the care of the one at UNC-Chapel Hill.
Long COVID: What We Know and What We Don’t Know
What We Know
It affects 10–30% of COVID patients. Symptoms can last weeks, months, or longer. Some people may never fully recover.
Symptoms can span across 10 organ systems.
Long COVID is a type of post-viral syndrome.
Post-viral syndrome can occur after infection with other types of viruses, including the flu.
What We Don’t Know
We can’t predict which COVID patients will suffer from it. Even mild or asymptomatic COVID patients may suffer from severe long COVID.
We can’t predict how long each patient will suffer from it.
We don’t yet understand why some people have some organ systems affected, and others have other systems.
Long COVID is more common and more often severe than post-viral syndrome from other common viruses. We don’t know why.
We’re not in the short rows yet. More than five dozen COVID recovery clinics have opened in hospitals and universities across the country, including the one at UNC. Some clinics study their patients, while all of them help coordinate and tailor care with experts in the multiple organ systems that could be affected by long COVID. They also help patients understand where their symptoms fall within the spectrum of the condition. The clinic helped me understand that I was suffering from a real condition and had not completely lost my mind.
As of this summer, I have had three appointments at the clinic and more are on the way. I have seen a long COVID specialist and a neuropsychologist through the clinic. I have had an MRI, X-rays, blood tests, urinalyses, extensive pulmonologist exams and multiple visits with my general practitioner. The clinic and my general practitioner work to fill in the blanks of my illness. They provide prescriptions to help mitigate these symptoms they can’t yet cure.
People are kind. There was a time in the early part of 2022 when I developed a stutter. I didn’t have a stutter as a child, but maybe you did, or maybe you have a stutter now. Maybe you know what it means to have the words for something in your brain but unable to get those words to come out of your mouth. You can see that it is frustrating for people trying to hear your words, too. You can see them try to fill in for you, or feel sorry for you as you work for two full minutes to say something profound, like, “It’s hotter today than it was yesterday.”
If you haven’t, just take it from me: It’s not awesome. My job is communication. I have always taken words for granted. Take this from me, too: People are kind. People are so kind. There was the day at the grocery store when I spent 30 seconds trying to ask the teenager working the checkout for paper bags. I couldn’t say paper bags, but I could say, “I’m sorry” after I realized there was a line behind me. I looked up at her and saw she was smiling at me. Not the pitying smile I’d gotten used to, but a smile of kindness. “Why are you sorry?” she said. “I’m right here with you.”
My daily experience has become punctuated by kindnesses. The mug of lilies left at my door by a beloved neighbor. The octogenarian couple who fixes supper for us each week for months. The person experiencing homelessness who checks in on my health when I was able to return to my early morning dog walks, who notices when I haven’t been sleeping or when I seem to be feeling better.
Whenever I feel out to sea, I am washed home on a river of kindnesses.
It takes a village, but some of us are on deserted islands. At one point, I struggled to make it from dawn to dusk — even with the following help: My parents drove from an hour away to play with my children and take me to places like the grocery store; my friends brought dinner; my business partner helped with my work; my husband took our children to school and managed the basic pieces of living; and a group of doctors probed around to see what is wrong with me.
I know that I am an exception when it comes to having a village. I live in a happy, walkable neighborhood filled with people I care about who help me. I have a husband, best friend and parents who set their own lives aside so that I may live mine. I have excellent insurance and can afford to bounce from doctor to doctor.
At my first visit to the long COVID clinic, I learned that my case is “moderate.” There are people who can’t get out of bed to brush their teeth. There are people who take their children to school or go to the grocery store and then can’t find their way home.

You never can tell what another person is going through. Since experiencing long COVID, I understand this saying in a whole new way. I don’t look sick, but sometimes I struggle to remember where I am, or I have a panic spiral because I don’t know where to sit at a restaurant, or I can’t read signs.
As an entomologist, I’m used to people telling me their secrets, whether they realize it or not. I can tell a lot about you from those roach pictures you send me or the ants you’re finding in your backyard. I can tell what frightens you, what delights you, how tidy your house is, what makes some of your dreams. I love these things about you.
Since long COVID entered my life, I’ve learned even more about others’ secrets. People call me with their fears and their maladies. Like my urge to share my health status at Thanksgiving, they’re trying to find someone to tell them what to do, or that they’ll be okay, or maybe they’re trying to be kind to me, to tell me it’s not all so bad, see?
Each of us has a lot going on that nobody can see.
Each of us has a lot going on that nobody can see. Our worries and our dreams are as important as the amount of space they take. The parent who can’t sleep because her child is getting bullied at school is as anguished as I am in my sleepless doom spirals, maybe more so. It takes a lot to be human.
Memory isn’t everything. I’ve come to see memory as a small bonus to the living experience. It’s nice to have, but it’s not always reliable. Take conversations with my brother about our childhood, for example, where he simply misremembers, replacing my character with our beloved, long-dead dog, Sadie.
“But how did Sadie scale the fence to jump the railroad tracks?!” I’ll say. “Only a person can do that! And where would I have been all these years of your adolescence?! It was me!”
“She was a remarkable dog,” he’ll reply, completely serious.
Now I battle with my own memory. It frightens me when someone I’ve never met approaches me and talks about our conversation last week. A heavy, cold, eerie feeling settles in my stomach when someone mentions people I know I am supposed to know but can’t think how.
A Recent Study
A recent study found that long COVID sufferers reported more than 200 symptoms. Shortness of breath and racing heart are common, and so is trouble with memory. Other symptoms aren’t as common, but are also not unusual, including numbness and tingling sensations and trouble with speech. Even the eyeball thing is explained by the mystery that is long COVID.
Though much is lost in terms of memory, fragments of experience, feelings and emotions remain. I can’t tell you everything my husband has done in the last six months, but I won’t forget his form beside me as I reach out in my hours of wakeful darkness because I am tired of being awake, and I’m probably a little bored, and I want someone to let me know that they know I’m there. I’ll poke him just enough to wake him halfway.
“Am I snoring?” he’ll say.
“No.”
“Is everything okay?”
“I’m just awake.”
“I can be awake, too.”
- Categories:



Great account Eleanor. I really hope you are feeling a lot better now. I’m also an entomologist with Long Covid, but getting much better after 8 months. I am still incredibly susceptible to cold and get flare ups (Mast cells?) which put me under a pile of blankets, but not half as bad as it was immediately post Covid.
Best eishes,
Ray Cannon
Eleanor, thank you for this informative and evocative testimony. I admire your courage and commitment in sharing your experience. May you soon know the fullness of life when this illness has become a bad memory.
Eleanor, I am so sorry that you have this experience of long COViD. Thank you for sharing it as it helps others to endure a time when they are temporarily lost to themselves, their family., and to their work.
Be especially good to yourself. You are greatly admired and loved. Love, Liz and Dave Meador
Your story is so enlightening. Thank you for sharing as it helps to understand the many ways covid effects different individuals. May you continue to improve.
This is one of the most amazing articles I’ve ever read. You gave a vivid description of Long Covid yet in the end I learned more about how tough it is to be human and incredible being a human is